NADIS reports of chronic copper poisoning are common during the late summer in pedigree Bluefaced Leicester and Texel ram lambs and shearlings which were being fed substantial amounts of concentrates.
Copper is one of the most frequently diagnosed inorganic poisonings of domestic ruminants. Two distinct syndromes are recognised: chronic copper toxicity which is commonly reported following long-term liver storage of dietary copper and acute copper toxicity which is occasionally reported following inaccurate administration of copper injections.
Chronic Copper Poisoning
Chronic copper poisoning occurs after the sheep's liver capacity for copper storage has been exceeded. This results in sudden release of copper into the circulation, causing liver damage, destruction of red blood cells and jaundice.
There is variation in breed susceptibility to copper toxicity related to ability to absorb dietary copper. North Ronaldsay, Texel, Suffolk and several continental short-wool breeds of sheep are relatively susceptible, when compared with, for example, Cheviots and Scottish Blackfaces. Growing lambs are more susceptible than adult ewes.
Clinical signs
The clinical signs associated with chronic copper poisoning are sudden in onset and affected animals become increasingly weak. Some sheep may spend time wandering aimlessly or head-pressing. As the disease progresses, jaundice develops and breathing becomes shallow and rapid due in part to the development of anaemia.

Fig 1 Urine often appears black due to red blood cell breakdown

Fig 2 Jaundice of the gums

Fig 3 Jaundice of the conjunctivae and third eyelid
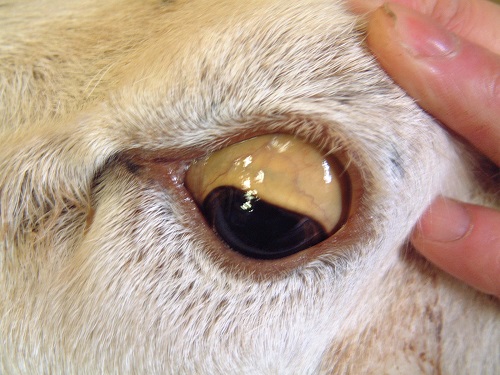
Fig 4 Jaundice of the sclera of the eye

Fig 5 Most animals die following a short period of recumbency. Note yellow coloured skin
The diagnosis of copper poisoning is based on the housing and feeding history, clinical signs and post-mortem findings of a pale tan to bronze-coloured liver and dark red or black kidneys. The diagnosis can be confirmed by laboratory identification of high kidney copper concentrations.

Fig 6 Bronze coloured liver

'Fig 7 'Gun Metal' appearance of the kidneys
Management of outbreaks of chronic copper poisoning
The treatment response to supportive therapy in animals showing clinical signs is poor. Resources should be directed towards identification of the underlying causes of the problem and the prevention of clinical disease in the remaining at-risk animals. This can be achieved by a programme of oral dosing or subcutaneous injection of ammonium tetrathiomolybdate to effectively 'strip' copper from the liver, although in recent months this has become prohibitively expensive other than for very valuable animals. Copper antagonists such as molybdenum or sulphur can be added to the ration to prevent further liver accumulation of copper. Your vet can provide more precise information about the management of copper poisoning in sheep.
Prevention of copper poisoning
Poisoning results from a combination of efficient absorption and high dietary availability of copper. Prevention depends on avoiding the feeding of copper-rich diets to susceptible animals. Sheep breed, age (young animals absorb copper very efficiently) and the presence of dietary copper antagonists such as iron, sulphur and molybdenum all influence the efficiency of absorption. The availability of dietary copper varies between different feeds. Feeds with high concentrations of available copper include -
- Pasture, silage and root crops grown on ground to which large quantities of pig or poultry manure has been applied.
- Distillery by-product feeds such as distiller's dark grains produced from copper stills. Concentrate feeds containing palm oil or molassed sugarbeet pulp. (Whole grain cereals are relatively poor sources of copper.)
- Other potential sources of copper include; access to cattle minerals; copper sulphate foot baths; and fungicide-treated timber.
In the highly susceptible North Ronaldsay breed of sheep, or in intensively-managed housed sheep, poisoning can result from prolonged feeding of diets with relatively low copper concentrations. Housed sheep should, therefore, not receive any form of copper supplementation before or during housing.



